In the United States, dizziness affects 35% of adults age 45 years and older. Physical therapists, audiologists, and ear, nose, and throat doctors are experts the medical profession turns to in diagnosing disorders of the vestibular system.
By Trent Tripp, PT, CEEAA
Balance is the ability to maintain the body’s center of mass over its base of support, and is achieved by a complex set of sensory systems that include visual, proprioceptive, and vestibular. Information gathered by these systems is processed and integrated by various centers in the brain which then produce motor output. A properly functioning balance system allows humans to see clearly while moving, identify orientation with respect to gravity, determine direction and speed of movement, and make automatic postural adjustments to maintain posture and stability in various environments. A dysfunction anywhere in the balance system leads to dizziness. Symptoms of dizziness include vertigo, which is an inaccurate perception of motion often feeling as if the room is spinning. Disequilibrium may describe a person’s dizziness while walking or standing, causing general or actual ataxia. Finally, light-headedness, or a “fish bowl effect,” is another more specific term for dizziness. Understanding what a person is feeling and getting a detailed characterization of their symptoms is significant in determining the etiology.1
Effects From Age 40 Years and Older
According to the American Physical Therapy Association Section on Neurology, dizziness affects 35% of adults aged 40 years and older in the United States, which corresponds to 69 million Americans. The odds of experiencing balance dysfunction increase significantly with age such that 85% of individuals aged 80 years and older have evidence of balance dysfunction. Not coincidently, this correlates to the incidence of falls with older adults. One in three adults over the age of 65 years will fall each year, and one-half of people over the age of 80 years will suffer a fall.2
It is estimated that 45% of individuals who seek medical care for complaints of dizziness have a vestibular dysfunction. Vestibular-related dizziness is associated with interruption of daily activities, sick leave from work, and avoidance of leaving the house when compared to non-vestibular causes of dizziness. The good news is that most people suffering from dizziness due to vestibular dysfunction can get better, thereby reducing their risk of falls and improving their quality of life.2
Inside the Vestibular System
The vestibular system is grossly divided into the peripheral vestibular system and the central vestibular system. The peripheral system consists of a set of motion sensors that send information about head angular velocity and linear acceleration to the central nervous system. The vestibular nuclear complex and the cerebellum process this information and combine it with other sensory information to calculate head and body orientation. The output of the central vestibular system goes to the ocular muscles and spinal cord to serve three important reflexes: 1) the vestibular ocular reflex (VOR), 2) the vestibulocollic reflex (VCR), and 3) the vestibulospinal reflex (VSR). From here, there are afferent motor neurons controlling eye movements and postural adjustments. The VOR generates eye movements that enable clear vision while the head is in motion, and while the VCR acts on the neck musculature to stabilize the head. The VSR generates compensatory body movement to maintain head and postural stability and thus prevent falls.
Lesions of the vestibular system can affect the peripheral vestibular system, the central system, or both. As stated above, the peripheral system consists of motion sensors inside the boney labyrinth. The central vestibular system is contained within the vestibular nuclear complex primarily in the PONS. The cerebellum is the adaptive processor which monitors vestibular performance and readjusts processing if necessary. As a sensor of gravity, the vestibular system plays an integral role in controlling posture and balancing the body.
[sidebar float=”right” width=”250″]Product Resources
The following companies offer technologies for vestibular rehabilitation and treatment of dizziness:
Biodex Medical Systems
www.biodex.com
Hoggan Scientific LLC
www.hogganhealth.net
Micromedical Technologies Inc
www.micromedical.com
Natus Medical Inc (NeuroCom)
www.onbalance.com
novel electronics
www.novelusa.com
Perry Dynamics Inc
www.perrydynamics.com[/sidebar]
Testing Technologies
When presented with a patient showing signs and symptoms of vestibular dysfunction, the physician may order a caloric test. This test is the best one for determining whether a vestibular dysfunction is peripheral or central and for identifying the side of the defect. This test is objective and quantifiable using recording instruments to measure the eye movements. In this test, each ear is irrigated for 40 seconds with cold water then warm water. The water stimulates or suppresses the sensory organs within the inner ear or labyrinth, causing an asymmetry between the right and the left organs. Under normal conditions, this stimulation would cause eye movements or nystagmus. An analysis of the nystagmus in each eye can determine whether the system is working normally or if there is a lesion of the sensory organs in one side. This test is quick and relatively inexpensive, but since the results of one ear are compared to the results of the other ear, it cannot detect bilateral vestibular loss. It also will not show the unilateral deficit if the central system has compensated to even out the two peripheral signals.3
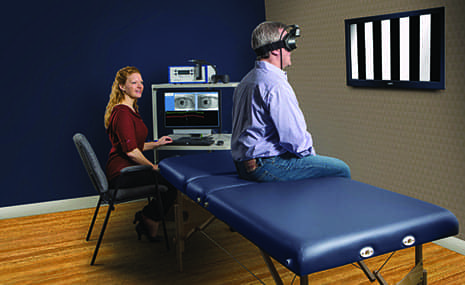
Rotary chair testing is another method to test the function of the labyrinth and the vestibular nerve. This test is done in a dark room also using recording devices to measure and analyze the eye movements. The rotational movements of the head caused by the rotation of the chair create sustained eye movements called nystagmus. These eye movements continue after the rotation is stopped, but they slow as time passes. Analyzing these eye movements can assess vestibular system function. This test is essential in diagnosing and quantifying bilateral vestibular dysfunction. It can also quantify central compensation, which is desirable in treating the negative effects of unilateral peripheral dysfunction.4
Rotational chairs are available from several manufacturers, including Micromedical Technologies Inc, Chatham, Ill, which offers the System 2000 line of rotational chairs. The System 2000 Auto-Traverse Rotational Vestibular chair includes a dark room enclosure, XY laser projector, and full-field optokinetic drum in addition to the ability to shift the center of rotation off-axis. The company also offers the System 2000 Reclining Rotational Vestibular Chair, which reclines to a caloric incline position as well as a supine position. The Nydiag 200 Rotary Chair from Interacoustics, Eden Prairie, Minn, is also designed to provide utility for rotational testing and double as a VNG exam table.
PTs’ Roles in Diagnosis and Treatment
Often dizzy patients will be referred to a PT directly from their primary care doctor with no laboratory test results. A PT’s diagnosis of the cause of the dizziness is made based on a thorough history including the signs and symptoms of the dizziness. A few questions that may be investigated include: “Is it vertigo, light-headedness, or disequilibrium? Does the patient’s vision become blurry with movement? Is the patient nauseous? What are the circumstances in which the dizziness occurs? How long do the symptoms persist once stimulated?” Understanding the tempo, the exact nature of the symptoms and the circumstances is an essential part of the PT evaluation.
Once the PT has completed the subjective portion of the exam, analyzing a patient’s eye movements can be the window into the vestibular system. Certain basic physiological testing to analyze eye movements are best done with fixation blocked using Frenzel goggles with an infra-red video system to record the eye movements. The camera systems can be binocular or monocular, and the picture is presented in real time on a screen. The session is also recorded so that it can be viewed several times if necessary.
Tests performed with fixation blocked include those where the therapist is looking for abnormal eye movements or nystagmus. Performing these tests in room light will allow the patient to fix his or her vision on a stationary object and suppress the eye movement. It is important for the therapist to analyze the nystagmus to detect the slow phase and the fast phase. The direction of the nystagmus is determined by the direction of the fast phase which will point towards the more active sensory organs in the peripheral vestibular system. Whether that is the dysfunctional side or not depends on which test the therapist is performing. When testing for unilateral hypofunction, the fast phase will point toward the healthy side. When testing for Benign Paroxysmal Peripheral Vertigo, the affected side will be the hyperactive side.
Assessing nystagmus among other abnormal eye movements is an important part of a PT’s ability to evaluate and diagnose many vestibular lesions. Using Frenzel goggles can make that assessment much more reliable, and several sources make these goggles available to the physical therapy market. Micromedical Technologies Inc offers its RealEyes xDVR video goggles, designed to be used during the Dix-Hallpike test for diagnosis of benign paroxysmal positional vertigo (BPPV). These goggles are also built for use during canalith repositioning for treatment of BPPV. Natus Medical Inc, San Carlos, Calif, offers VideoStar Frenzel goggles, for use in BPPV therapy.
In the case where a patient has been referred to the PT and the vestibular functional deficit is unclear, referring to an ENT or audiologist for laboratory assessment, including rotational chair test and caloric testing, can confirm a diagnosis even if central compensation has occurred. PTP
Trent Tripp, PT, CEEAA, graduated from the University of Kansas in 1999. He has worked at HealthSouth Valley of the Sun Rehabilitation Hospital as a physical therapist since 2007. Tripp is a LSVT BIG Certified therapist, and a Certified Exercise Expert for Aging Adults given by Academy of Geriatric Physical Therapy. He has advanced education including Vestibular Rehabilitation: Theory, Evidence and Practical Application at Rehabilitation Institute of Chicago and The Emory University Vestibular Rehabilitation: A Competency Based Course given at the University of Southern California in 2013. For more information, contact [email protected].
References
1. Vestibular Rehabilitation. Theory, Evidence and practical Application. Rehabilitation Institute of Chicago. Chicago. Course given March 7-9, 2013.
2. Agrawal Y, Ward BK, Minor LB. Vestibular dysfunction: prevalence, Impact, and need for targeted treatment. J Vestib Res. 2013;23(3):113-117.
3. Herdman SJ. Vestibular Rehabilitation. 3rd Ed. Philadelphia. F.A. Davis Company; 2007.
4. Vestibular Rehabilitation-A Competency-Based Course. Emory University, University of Southern California & APTA. Los Angeles. Course given July 15-20, 2013.