Robotic rehabilitation technologies help patients move and practice functional tasks with confidence and intensity
Robotic technologies used throughout healthcare continue to grow in popularity, and in physical therapy their ability to facilitate mass repetition and increase safety for the patient attracts considerable interest. These types of clinical benefits provided by robotic devices have been fully embraced by Madonna Rehabilitation Hospitals, which has facilities located in the Nebraska cities of Lincoln and Omaha. To understand the actual performance these devices deliver, three of Madonna’s physical therapists share vignettes about how robotic technologies helped advance patients toward their rehab goals.
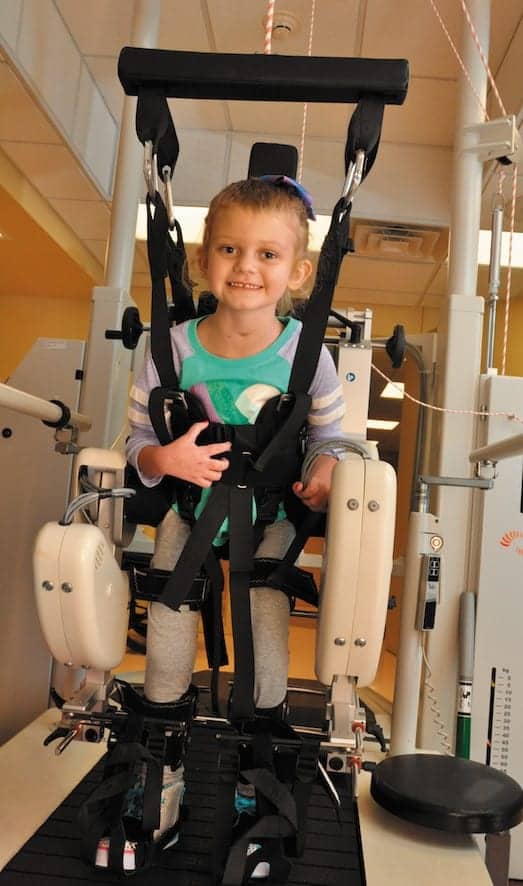
The Therapist’s Little Helper: Pediatric Lokomat
By Sarah Economides, PT, DPT, PCS
Hayden is a 5-year-old girl who suffered a severe traumatic brain injury when she was involved in a high-speed car accident on July 19, 2018.
Hayden spent 6 weeks in intensive care, had a tracheostomy placed with mechanical ventilation, and was dependent on tube feeding through a gastronomy (G) button for nutrition. She admitted to the pediatric unit at Madonna Rehabilitation Hospitals in Lincoln, Neb, on August 30, 2018. Hayden was completely dependent for all mobility, unable to initiate movement or follow commands. She had severe tremors affecting her left arm and leg, couldn’t speak or eat, and had significant weakness, along with increased tone and spasticity, in her arms and legs but primarily on her right side.
Within a week, Hayden was fitted in the Hocoma Pediatric Lokomat from Norwell, Mass-headquartered Hocoma. The Pediatric Lokomat is a partial body weight support treadmill training device that utilizes a robotic orthosis to assist with consistent reciprocal stepping movements to promote a normal gait pattern.
One benefit of using the Lokomat is that patients can get up and move much sooner than without the device because they are in a safe and secure position and don’t require as much support or facilitation from therapists. Using the Lokomat also allowed Hayden to increase her endurance and strength while retraining her body in a normal movement pattern for gait activities at a much higher rate of repetition than facilitating gait on the ground. Patients can be provided a wide variety of assistance, variable body weight support, and different speeds to constantly challenge and progress their ambulatory mobility. Over the course of her 8 weeks in inpatient rehabilitation, Hayden used the Lokomat two to three times per week for initial progression of head and trunk control and help with transfers, and eventually focused on gait training for working toward independent mobility and return to school and age-appropriate activities.
Hayden initially required 100% support from the Lokomat and even needed an additional chest strap and occasional facilitation for head control to help her stay in an upright position. On land, she needed maximal to dependent assist to ambulate a few feet with constant facilitation for weight shifting, upright posture, and scissoring gait pattern with knee hyperextension/plantarflexion synergy patterns. Within five sessions of Lokomat training Hayden had progressed to moderate assist with ambulation on land and was fitted with custom hinged dynamic ankle foot orthoses (DAFOs) to promote optimal foot/ankle positioning and decrease tone for better standing balance and leg control.
After 12 sessions of training, Hayden stood to don the harness instead of sitting, had decreased significantly the amount of orthosis assistance, and ambulated with minimal assist with AFOs on land. Upon discharge, Hayden had completed 20 sessions in the Lokomat and progressed significantly. The robotic orthosis was no longer necessary to guide her movement since she could control her legs in a safe and coordinated walking pattern for longer distances with only hand-held assistance.
Today, Hayden is a happy and healthy first grader who continues to make amazing progress post-injury. She continues to receive occupational and speech therapy for higher-level cognitive function and school access. Hayden graduated from physical therapy and now she runs, jumps, and dances independently and without DAFOs because of the intense rehabilitation and Lokomat training she received early in her recovery.
Sarah Economides, PT, DPT, PCS, earned a Doctorate of Physical Therapy from Creighton University in Omaha, Neb, in 2010 and completed a pediatric physical therapy residency at Creighton in 2011. Economides has been a board-certified pediatric specialist in physical therapy since 2014. She has been employed by Madonna Rehabilitation Hospitals for the past 8 years and works in an inpatient rehabilitation setting primarily with children 0-18 years of age.
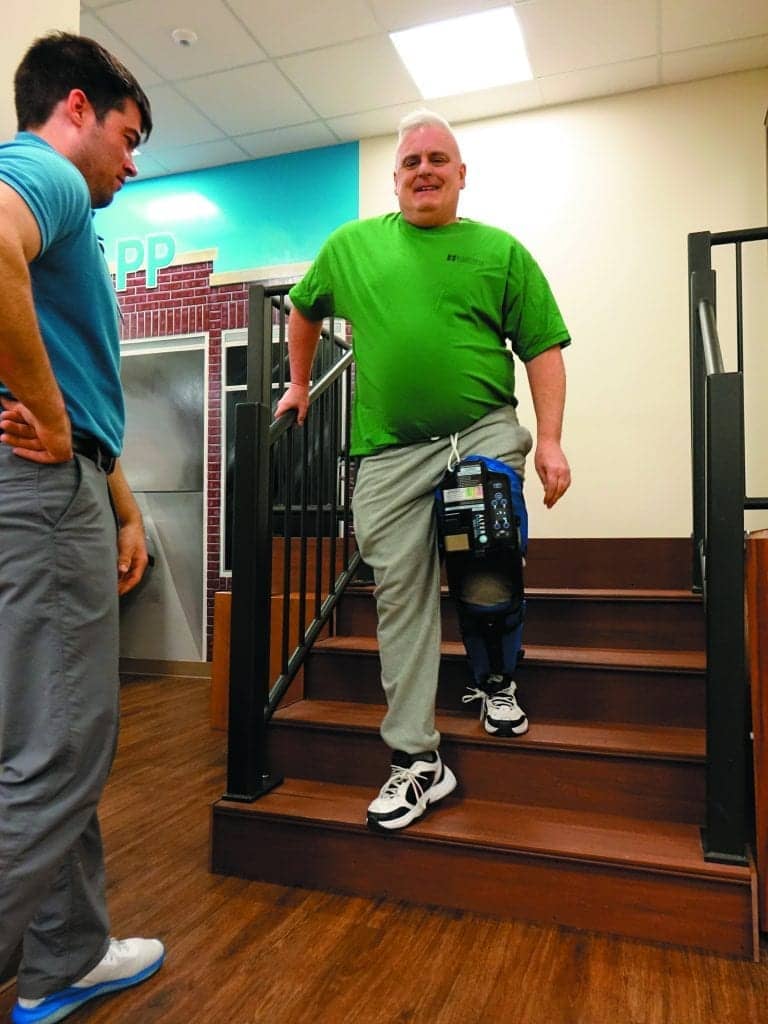
Powering Up Functional Mobility with the AlterG Bionic Leg
By Amy M. Burggraff, PT, DPT, CBIS
Following a significant injury and surgery to repair his left quadriceps, PJ chose Madonna Rehabilitation Hospitals in Omaha, Neb, for his skilled outpatient rehabilitation. As PJ worked to restore normal strength and function, it became evident that he did not have the confidence or the strength to complete tasks requiring eccentric control, such as the stairs. At this point in his recovery, the AlterG Bionic Leg, manufactured by AlterG Inc, Fremont, Calif, was incorporated into his plan of care.
The AlterG Bionic Leg is a wearable lower extremity orthosis that provides assistance to users during specific functional mobility tasks over the course of their rehabilitation. The AlterG Bionic Leg is a battery-powered portable device that offers customized range of motion and assistance to patients with decreased muscle strength and sensory awareness on an affected side. The device is untethered and provides powered assistance through patient-initiated movement to complete functional mobility training within a clinical setting.
The AlterG Bionic Leg provides robotic assistance for knee extension during both concentric and eccentric demands of a functional mobility task. By adjusting the assistance with concentric muscle demands and resistance with eccentric muscle demands, the therapist can customize the device to a patient’s individual needs. These properties allow the clinician to provide cuing and/or hands-on facilitation elsewhere in order to restore normal movement patterns. Additionally, the device restores patients’ confidence with functional mobility tasks by providing the appropriate amount of assistance to keep them safe as well as challenge them. The device is appropriate for patients following stroke, traumatic brain injury (TBI), incomplete spinal cord injury (SCI), and any other neurologic conditions that may affect muscle strength and sensory awareness, which ultimately impacts their functional mobility. The AlterG Bionic Leg is also appropriate for orthopedic conditions affecting knee extension strength. This includes, but is not limited to, total knee replacement and quadriceps tendon injury.
For individuals such as PJ, the AlterG Bionic Leg was instrumental in improving stair negotiation following a quadriceps tendon repair. Following his injury, PJ had difficulty restoring full quadriceps strength secondary to the type of repair. This led to significant difficulty with eccentric quadricep control, which impacted his ability to negotiate stairs.
Prior to using the AlterG Bionic Leg, PJ demonstrated significant compensations through his hip and back due to decreased confidence on his affected side. After introducing the AlterG Bionic Leg with the appropriate amount of resistance and assistance, PJ demonstrated correct body mechanics with stair negotiation and improved confidence both in and out of therapy. The ability to complete mass repetition of a correct movement pattern through use of the AlterG Bionic Leg facilitates neuroplasticity in order to restore a normal movement pattern. Upon completion of skilled physical therapy, PJ was able to complete stair negotiation with a reciprocal pattern and minimal to no compensation thanks to the AlterG Bionic Leg.
Amy M. Burggraff, PT, DPT, CBIS, earned a Doctorate of Physical Therapy from the University of Colorado Anschutz Medical Campus and completed undergraduate studies at the University of Nebraska-Lincoln. Burggraff is currently employed at Madonna TherapyPlus Omaha. She works with individuals diagnosed with mild traumatic brain injury/concussion, traumatic brain injury, spinal cord injury, stroke, Parkinson’s disease, and other neurological conditions. She is a certified brain injury specialist and LSVT BIG trained clinician.

Taking a Cue with the EksoGT
By Marin Salisbury, PT, MPT, CBIS
Icy roads on a cold day in February 2018 prevented Megan from stopping at a red light. Her car slid into an intersection and was struck by an approaching semi-truck. She suffered a severe traumatic brain injury, leaving her with spastic right hemiparesis. Megan slowly regained consciousness during her inpatient stay at Madonna Rehabilitation Hospitals in Lincoln, Neb. Her physical therapist began addressing her gait and mobility skills. However, Megan’s ataxia, spasticity, and right-sided weakness made over-ground walking extremely difficult.
She was recommended as a good candidate for using the EksoGT exoskeleton from EksoBionics, Richmond, Calif. At the time of her initial fitting for the Ekso, Megan was walking up to 100 feet with a quad cane and minimal assist of two therapists. She continued using the Ekso for several more sessions during the remainder of her inpatient rehabilitation. Megan transitioned to Madonna TherapyPlus, an outpatient program where her therapist continued to incorporate the technology into her plan of care.
The EksoGT is a robotic gait orthosis that allows over-ground, full weight-bearing gait training with robotic assistance, providing proper step sequence, postural support, and the ability for therapist cuing and facilitation. This model also includes an option to adjust the level of robotic assistance from both legs to one leg, to neither leg, while still offering stance and postural control.
When robotic assistance is provided to the patient, the Ekso can be adjusted and allow the patient the freedom to use his or her own volitional motor control while the robotics prevent spasticity, ataxia, and postural weakness from negatively affecting the gait pattern. For therapists, there are multiple ways to offer tactile and verbal cues that allow the patient to sense what changes need to be made to maximize gait mechanics efficiency.
Megan continues to regain her independence in outpatient therapy. She is a community ambulator, using a wheeled walker and beginning to transition to a lesser assistive device. Megan has progressed significantly in her weekly Ekso therapy session. She begins the session in full robotic mode, practicing proper step length, height, and timing. The therapist has the option of switching to the 2Free mode, shutting off the robotics for both legs, and Megan is cued to control her steps, practicing the motor skills she just worked on with the robotic assist.
Spasticity continues to limit Megan’s speed, but she is regaining motor control and no longer struggles with ataxia. Megan credits the Ekso with helping her learn “real walking.” She feels safe and confident with the technology supporting her foot and knee and has no fear of stumbling.
Nearly 20 months postinjury, Megan walks for 30 to 45 minutes in the Ekso over ground, with good sequence and mechanics, providing the repetition she needs for continued progress. PTP
Marin Salisbury, PT, MPT, CBIS, earned a Masters in Physical Therapy from Des Moines University, Des Moines, Iowa, after completing undergraduate studies at Saint Cloud State University in St. Cloud, Minn. She has been an outpatient neurological physical therapist at Madonna TherapyPlus Lincoln for more than 13 years. She is a certified brain injury specialist and a certified lymphedema therapist. For more information, contact [email protected].

A Lighter Load for Intensive Rehab
By Frank Long, Editorial Director, Physical Therapy Products
Individuals whose walking has been impaired as the result of stroke, spinal cord injury (SCI), or traumatic brain injury (TBI) may need assistance on several dimensions as they attempt to recover the ability to walk. Among these tasks a therapist may be called to help with the patient’s balance support or assist with movements that promote mass repetition. Tasks such as these can strain a therapist physically and occupy time that might otherwise be spent with another patient. Technology that can help ease these demands is precisely the work for which the Intelligently Controlled Assistive Rehabilitation Elliptical (ICARE) by SportsArt, Mukilteo, Wash, is designed.
Assist As Needed
Patients looking to bring back their walking ability to its highest possible level will likely find part of their therapy will require them to perform a seemingly countless number of step-like movements aimed at building lasting gains in neuroplasticity. The activity of these movements can tax both patient and therapist. To ease those demands, the ICARE is engineered to provide assistance similar to what a therapist might offer: a physically and intuitively “assist as needed” approach during gait training.
Technology Roots in Rehab
SportsArt partnered in the development of this motorized elliptical trainer with Judith M. Burnfield, PhD, PT, Director of the Institute for Rehabilitation Science and Engineering, Director of the Movement and Neurosciences Center and the Clifton Chair in Physical Therapy and Movement Sciences at Madonna Rehabilitation Hospital. The insights generated by this partnership led the ICARE engineering team to build a device that provides leg movements that closely mimic the kinematic and electromyographic (EMG) patterns of walking. Other important therapeutic functions built into the ICARE include 40 levels of resistance to provide expansive customizability and a pedal cushioning system that facilitates a comfortable workout. The ICARE is also outfitted with an infrared safety system, fingertip controls, a variable unweighting harness, and an optional wheelchair ramp.
ICARE training can help individuals regain or retain the flexibility and strength required for walking, particularly if the muscle demands are customized to those with weakness during rehab. The ICARE was developed with a special focus on making the appropriate levels of assistance available to users so they might accomplish the required repetitions—both with partial body weight support and motor-assistance from the device’s footplates.
ICARE and the Evidence
Several studies in the academic literature report the performance of ICARE and its use in the study of gait recovery, fitness, and other rehabilitation-related topics. Among these are recent studies led by Burnfield in publications such as Pediatric Physical Therapy, Rehabilitation Psychology, The American Society of Mechanical Engineers Journal of Medical Devices, Cardiopulmonary Physical Therapy Journal, and others. PTP





