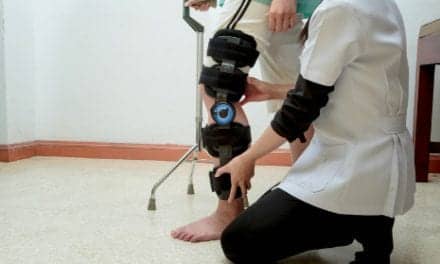
Advanced technologies are used throughout the continuum of care to address gait and balance retraining. One device therapists use, the Ekso GT (pictured above), provides real-time feedback with the ability to adapt throughout a training session to tailor to a patient’s specific rehabilitation needs.
By Mollie Hope, PT, DPT, CBIS, and Abby Albers, SPT
Madonna Rehabilitation Hospitals in Lincoln and Omaha, Nebraska, provide rehabilitation for adults and children, specializing in the rehabilitation of individuals with traumatic brain injury, spinal cord injury, stroke, degenerative neurological conditions, and pulmonary conditions. This article provides an overview of how Madonna’s team of specialized therapists and researchers use advanced technology in the services they provide across the continuum of care to help each patient achieve his or her highest level of independence.
Gait and Balance Equipment Profile
Physical therapists at Madonna regularly utilize specialized equipment for gait and balance retraining. Available technologies include body weight support gait training systems, overground robotic gait devices, and computerized balance equipment. High repetition, intensity of training, and task specificity are some of the most important principles to drive neuroplasticity when working with individuals with neurological injuries or disorders.1 Using body weight support and robotic locomotor training devices to recover gait function, across the continuum of care, allows physical therapists to increase the duration and intensity of training. Additionally, this equipment reduces the need for the labor and staffing-intensive assistance often required in traditional methods of gait and mobility training. Body weight support systems can also increase safety for patients and therapists during standing and stepping tasks.2-4

The ICARE offers the clinician the option to utilize body weight support or use the device without body weight support, depending on the patient’s abilities, while allowing the patient to utilize kinematics similar to walking. The device allows the clinician to set a consistent minimum pace to help increase gait speed while allowing the patient to pedal above the motor speed, if able.
Body weight support gait training technologies are an important part of the equipment installed at Madonna. Among these devices are the Lokomat from Hocoma, Norwell, Mass, as well as the Madonna ICARE by SportsArt, Mukilteo, Wash an intelligently controlled assistive rehabilitation elliptical. Therapists at Madonna also use the body weight support treadmill system from Robomedica Inc, Mission Viejo, Calif, as part of the rehabilitation toolkit. At other facilities across the country there has been an emergence of devices that offer advanced treadmill or step function features. Among them is the DST8000 Triple Pro Dynamic Stair Trainer from Clarke Health Care Products, Camarillo, Calif. This device has electronically elevating steps and can be equipped to record session data.
Madonna’s therapists have several other types of equipment on-site that help measure and assess patient impairment, such as the Proprio 4000 from Perry Dynamics, Decatur, Ill; a reactive balance system that can be used for balance training. The Ekso GT from Ekso Bionics, Point Richmond, Calif, and Indego exoskeleton from Parker Hannifin, Cleveland, are two other devices that provide Madonna’s therapists advanced tools for overground robotic gait training.
To build a detailed evaluation of gait that includes objective measures of gait, Madonna’s Institute for Rehabilitation Science and Engineering utilizes the GAITRite walkway system from Franklin, NJ-based CIR Systems Inc, for gait analysis during research. This device can compute more than 90 measurements, including all the standard measures (cadence, velocity, step length, stride length, etc), in addition to many symmetry measures. There are other devices in the rehab marketplace designed to provide objective gait and balance analysis, which are in use at other facilities. Among those options are the Zeno Walkway from ProtoKinetics, Havertown, Pa, which can be used for clinical trials and research as well as clinical decision-making.

Using body weight support and overground robotic gait training technologies in conjunction with traditional physical therapy can be an effective way to increase intensity and repetition of gait training to drive neuroplastic change.
Intelligent Equipment for Effective Outcomes
Two patients with neurological injuries who used specialized equipment to improve gait independence and efficiency during their physical therapy treatment in Madonna’s Rehabilitation Day Program will be discussed. The Ekso GT will be highlighted with an individual with an incomplete spinal cord injury, and the Madonna ICARE will be highlighted with an individual with a middle cerebral artery (MCA) stroke.
The Ekso GT helps patients relearn optimal gait mechanics by incorporating active weight shifting to advance each step and lessening compensatory behaviors through guided stepping. Promoting correct biomechanics and mobility via a supportive exoskeleton reduces the need for support from the physical therapist when gait training overground and may allow the patient to more effectively rehabilitate his or her gait mechanics with greater repetition and intensity than traditional gait training. The Ekso GT also provides real-time feedback with the ability to adapt throughout a training session to tailor to a patient’s specific rehabilitation needs. The Ekso GT has been shown to significantly increase gait speed outside of the device after training in individuals with incomplete spinal cord injury.2,5,6
The ICARE offers the clinician the option to utilize body weight support or use the device without body weight support, depending on the patient’s abilities, while allowing the patient to utilize kinematics similar to walking.7 The intelligent motor allows the clinician to set a consistent minimum pace to help increase gait speed while also allowing the patient to pedal above the motor speed, if able. The stride length can be adjusted to optimize mechanics for each patient. The ICARE also offers several upper extremity support options, including dynamic handles and several different positions for stationary support. This allows the clinician the ability to customize upper extremity positioning to facilitate improvements in strength, range of motion, and attention to the upper extremities.
[sidebar float=”right” width=”250″]Product Resources
The following companies offer products that can be used for assessment and rehabilitation of gait and balance:
Accelerated Care Plus
www.acplus.com
APDM
www.apdm.com
Allard USA Inc
www.allardusa.com
Biodex
www.biodex.com
Clarke Health Care Products
www.clarkehealthcare.com
GAITRite/CIR Systems Inc
www.gaitrite.com
Gorbel Inc-Medical Division/SafeGait
www.safegait.com
Hocoma
www.hocoma.com
ICARE (SportsArt)
www.gosportsart.com
Mobility Research
www.litegait.com
OPTP
www.optp.com
Perry Dynamics
www.perrydynamics.com
ProtoKinetics
www.protokinetics.com
Tekscan
www.tekscan.com
Therapeutic Industries
www.therapeuticindustries.com
Vista Medical
www.boditrak.com[/sidebar]
Case study 1: incomplete spinal cord injury
Patient history
The patient is a 38-year-old male who sustained a C6 ASIA D incomplete spinal cord injury from a motor vehicle accident. He suffered a C6-C7 vertebral fracture, C2 body fracture with dislocation, and subsequent C4-T1 cervical spine fusion with halo device placement. The patient received rehabilitation in his home community and then 3 additional weeks of inpatient rehabilitation at Madonna prior to beginning outpatient therapy. The patient’s halo device was removed during his inpatient rehabilitation stay. He was able to walk short distances with a walker, but utilized a manual wheelchair as his primary mode of mobility. His past medical history included depression and insomnia.
Initial evaluation
Lower extremity strength and endurance
Manual muscle testing was performed on the patient’s bilateral lower extremities. His right lower extremity was globally weaker than the left lower extremity with hip flexion and extension graded 3/5, hip abduction 2/5, knee flexion 3/5, knee extension 5/5, plantarflexion 2+/5, and dorsiflexion 4/5. His left lower extremity grades were 4/5 except for 3/5 hip abduction, 5/5 knee extension, and 2+/5 plantarflexion. The patient completed the Five Times Sit To Stand test in 21.17 seconds. He was able to perform 3.5 minutes of continuous pedaling on the ICARE with constant motor assist at 25 strides per minute prior to fatigue.
Functional mobility
The patient was modified independent with transfers including floor transfers. His primary mode of mobility was with an ultra lightweight manual wheelchair, which he performed independently. He ambulated up to 200 feet with standby assistance using a front-wheeled walker. He was able to negotiate eight stairs with one handrail and contact guard assist.
Gait capacity and speed
Overground gait speed and endurance were assessed using the 2-minute walk test. His initial test distance was 135 feet using a front-wheeled walker, indicating a gait speed of 0.34 meters/second (m/s). This gait speed is indicative of a household ambulator and increased risk for falls.
Interventions
The patient participated in physical therapy five times per week for 8 weeks. Therapy included use of the Ekso GT, ICARE, and Proprio 4000, as well as participation in traditional balance training, strength training, and overground gait training. He completed robotic gait training on the Ekso two times per week for 5 weeks for a total of 10 sessions, performed four sessions on the ICARE, and then progressed to training on a traditional treadmill for three sessions prior to discharge.
Final outcomes
Lower extremity strength and endurance
Following 8 weeks of intervention, the patient improved his Five Times Sit to Stand score from 21.17 seconds to 14.52 seconds. Manual muscle testing was not reassessed prior to discharge.
He was able to perform 10 continuous minutes of pedaling on the ICARE with intermittent motor assist at 30 strides per minute prior to fatigue.
Functional mobility
After 8 weeks of intervention, the patient was able to complete all transfers independently without an assistive device. The patient progressed to being independent with ambulation using a front-wheeled walker for distances greater than 1,000 feet to navigate community environments such as the grocery store and shopping mall, and was also able to ambulate shorter distances without an assistive device with standby assistance. He was able to negotiate 32 stairs with one handrail independently.
Gait capacity and speed
His gait speed and endurance were reassessed using the 2-minute walk test utilizing a front-wheeled walker and with no assistive device. The patient walked 288 feet with a front-wheeled walker, indicating a gait speed of 0.73 m/s, which is a 0.39 m/s increase from his initial gait speed. He was able to walk 203 feet without an assistive device with a gait speed of 0.52 m/s. His final gait speed with and without an assistive device are indicative of a limited community ambulator.
Case study 2: Right MCA stroke
Patient history
The patient is a 60-year-old female with a right MCA stroke. She initially presented with left-sided numbness, significant upper extremity weakness, moderate lower extremity weakness, dysphagia, and left hemispatial neglect. She received 3.5 weeks of inpatient rehabilitation at Madonna prior to starting outpatient therapy. At initial evaluation in the Rehabilitation Day Program she ambulated using a tripod cane and continued to demonstrate significant left hemispatial neglect. Her past medical history included asthma, diabetes type II, hypertension, and hyperlipidemia.
Initial evaluation
Lower extremity strength and endurance
Manual muscle testing was used to assess lower extremity strength. Her left lower extremity was graded 4/5 strength globally and right lower extremity demonstrated 5/5 strength. She was initially able to complete 1.5 minutes of continuous pedaling at
27 strides per minute with motor assist on the ICARE prior to fatigue.
Balance
The patient completed the Berg Balance Scale with a score of 47/56. She also completed the Functional Gait Assessment with a score of 15/30, indicating an increased risk of falling.
Functional mobility
The patient required supervision for transfers due to left hemispatial neglect. Her primary mode of mobility was ambulation with a tripod cane with standby assist for management of her neglect. She was able to consistently ambulate for distances greater than 500 feet. She negotiated 15 stairs with single handrail and contact guard assist.
Gait capacity and speed
The Six Minute Walk Test was utilized to assess gait speed and endurance. She ambulated 684 feet using a tripod cane, indicating initial gait speed of 0.58 meters per second. This gait speed is indicative of a limited community ambulator.
Interventions
The patient participated in therapy four times per week for 8 weeks. Therapy included use of the ICARE and Proprio 4000 as well as traditional balance training, strength training, and traditional gait training overground without an assistive device. She completed 11 sessions on the ICARE and 16 sessions on the Proprio 4000.
Outcomes
Lower extremity strength and endurance
Following 8 weeks of intervention, the patient was able to pedal for 6.5 minutes continuously on the ICARE without motor assist. Manual muscle testing was not reassessed.
Balance
After 3 weeks of intervention, the patient scored 54/56 on the Berg Balance Scale. After 8 weeks she scored 24/30 on the Functional Gait Assessment, indicating a reduction in fall risk.
Functional mobility
After 8 weeks of intervention, the patient was independent with all transfers and gait with a tripod cane. She was also able to walk household distances without an assistive device independently. She was able to negotiate 20 stairs with a single handrail with supervision.
Gait capacity and speed
The patient was reassessed using the Six Minute Walk Test. She walked 1,156 feet with a gait speed of .98 m/s. This is an improvement from
initial evaluation of 0.4 m/s and indicates community level ambulation.
Conclusion
Utilizing body weight support and overground robotic gait training technologies in conjunction with traditional physical therapy can be an effective way to increase intensity and repetition of gait training to drive neuroplastic change. The use of technology can increase patient safety and confidence, help therapists mobilize patients earlier, and decrease the physical labor required from therapists. PTP
Mollie Hope, PT, DPT, CBIS, is an outpatient neurological physical therapist at Madonna Rehabilitation Hospitals, Lincoln, Neb. Hope earned her Doctor of Physical Therapy from Duke University, and was a neurologic physical therapy resident at Creighton University, Omaha, Neb. She is a certified brain injury specialist.
Abby Albers, SPT, is a third year DPT student at Midwestern University (AZ), and Madonna Rehabilitation Hospitals. For more information,
contact [email protected].
References
1. Merzenich M, Nahum M, Lee H. Principles of Neuroplasticity-Based Rehabilitation. Progress in Brain Research. Changing Brains: Applying Brain Plasticity to Advance and Recover Human Ability. Volume 207. Oxford, UK: Elsevier; 2013: pg 145.
2. Bonatti E, Baroncini I, Nalon C, et al. Locomotor training with exoskeleton EksoGT in patients with incomplete motor spinal cord injury in a hospital setting preliminary results. Poster presentation. ISCoS Meeting; September 16, 2016.
3. Hornby TG, Zemon DH, Campbell D. Robotic-assisted, body-weight-supported treadmill training in individuals following motor incomplete spinal cord injury. Phys Ther. 2005; 85:52-66.
4. Ramanujam A, Cirnigliaro CM, Garbarini E, Asselin et al. Neuromechanical adaptations during a robotic powered exoskeleton assisted walking session. J Spinal Cord Med. 2017 April 20:1-11.
5. Forrest G. Platform Presentation. ACRM Meeting; November 2, 2016.
6. Kern M, Chang S-H, Jennings J, Davis M, Francisco G; TIRR SCI Clinical Exoskeleton Group. Improving gait performance after SCI: a comparison between conventional PT and therapy using exoskeletons. Poster presentation. ASIA Conference, 2015.
7. Burnfield JM, Shu Y, Buster TW, et al. Comparison of lower extremity electromyographic (EMG) demands during ICARE training and walking. American Society of Biomechanics 2010 Annual Meeting.