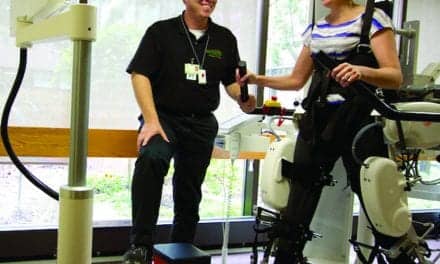
Body weight support devices are available for use over a treadmill or overground. Patients who use these devices are often less fearful and more motivated knowing they are safely supported and not at risk of falling.
By Jessica Finnegan, PT, MPT, NCS
This is an exciting time in the world of neurologic physical therapy. Rehabilitation technologies are emerging and research is ongoing to determine the efficacy of these products. In the current healthcare environment, rehabilitation stays are becoming shorter and physical therapists (PTs) must find a way to prioritize which interventions will be most beneficial to their patients. This article discusses several rehabilitation technologies with the hope of helping PTs integrate them into their plans of care to improve mobility in patients recovering from stroke and other neurological disorders.
Convenience, Safety, and Early Mobility
Intensive, repetitive mobility-task training is recommended for all patients with impaired gait after stroke.1 In the past, mobilizing a patient with dense hemiparesis may have required two to three skilled therapists. This has obvious implications for staff efficiency and productivity. In addition, musculoskeletal injuries are commonly reported by healthcare providers and are often associated with manual patient handling.2 Workplace injuries can be a threat to the health and careers of PTs and should be avoided. Darragh and colleagues explored physical and occupational therapists’ experience with safe-patient-handling (SPH) equipment, such as ceiling lifts, floor lifts, and more. This equipment is becoming more widely available, allowing early mobilization of patients with fewer skilled staff members present and reduced risk of injury to the therapist. In this study, therapeutic uses of SPH equipment included transfer training, functional ambulation, and bed mobility.
Therapists also reported using SPH devices to address impaired attention, visual perception, and neglect. Overall, therapists who used SPH equipment “experienced increased options in therapy, accomplished more, and mobilized patients earlier in their recovery.” They also remarked that they needed to co-treat or solicit help from other professionals less frequently, which should improve productivity overall.3
[sidebar float=”right” width=”250″]Product Resources
The following companies also provide products to treat mobility impairments and neurological rehabilitation:
Allard USA Inc
www.allardusa.com
Aretech
www.aretechllc.com
Bioness
www.bioness.com
Clarke Health Care Products
www.clarkehealthcare.com
GAITRite/CIR Systems Inc
www.gaitrite.com
Gorbel Inc-Medical Division/SafeGait
www.safegait.com
Hocoma Inc
www.hocoma.com
Mobility Research
www.litegait.com
ProtoKinetics
www.protokinetics.com
Solo-Step
www.solostep.com
Tekscan
www.tekscan.com
Vista Medical
www.boditrak.com[/sidebar]
Body Weight Support
One example of a safe-patient-handling device that can be used for functional ambulation training is the LiteGait from Mobility Research, Tempe, Ariz. LiteGait allows the therapist to raise the patient to standing using an electronic control. Once upright, the therapist can adjust the amount of weight that is supported through the device’s overhead harness. It can be used for gait training over a treadmill or overground.4 Products such as LiteGait allow the therapist to prioritize the patient’s gait pattern, rather than being limited by the therapist’s own capacity to hold the patient upright. Because the patient is secured in the harness, the therapist’s hands are free for more therapeutic purposes, such as facilitation of weight shift or limb advancement. Patients are often less fearful and more motivated knowing they are safely supported and not at risk of falling. The device’s mobile base means the treatment is not limited to areas below a ceiling track, as is the case with other devices. This allows the therapist to customize treatment to each patient’s home environment and individual goals—eg, walking into the bathroom, reaching into closets and cabinets, etc. Darragh et al reported, however, some therapists in their study preferred the maneuverability of ceiling lifts when compared to floor lifts.3
The ability for a patient to use a harness for body weight support during therapeutic activity is available in products offered by several manufacturers. The Vector Gait and Safety System from Valencia, Calif-based Bioness features a ceiling-mounted trolley operating on an overhead track that attaches to a harness and provides body weight support in addition to preventing falls. The SafeGait 360° Balance and Mobility Trainer from Gorbel Inc-Medical Division, Fishers, NY, is built to provide safe patient handling in an overhead rail design. This body weight support system attaches to the SafeGait Embrace Harness, designed to optimize patient comfort. Another manufacturer, Ashburn, Va-based Aretech, offers the ZeroG Gait and Balance Training System as a device that can assist in treating a wide range of diagnoses. ZeroG’s robotic trolley operates on an overhead track and uses a touchscreen or wireless remote user interface. Solo-Step, North Sioux City, SD, offers its Solo-Step body weight support system in a ceiling-mounted track design as well as a portable system that can be used outdoors overground.
Treadmill Training
There is evidence that cardiorespiratory training, including treadmill walking and stationary cycle ergometry, has many benefits during stroke recovery. “Exercise training improves functional capacity, the ability to perform activities of daily living, and quality of life, and it reduces the risk for subsequent cardiovascular events.”5 Treadmill training (with or without body-weight support) can improve cardiovascular fitness and walking ability in subacute stroke.5 While treadmill training is clearly beneficial, it can be difficult to implement with lower-level patients. Even with the use of body weight support, the therapist may become fatigued when providing the physical assistance required for stepping. This fatigue may then limit repetitions, which are essential for motor learning.
A recent study by Russo and colleagues researched the use of a robotic exoskeleton for gait training in acute stroke patients. This study found that the use of a robotic exoskeleton allowed significantly more repetitions of stepping than did traditional PT. They found significantly higher gains in Functional Independence Measure motor scores in the treatment group, but no difference in discharge destination.6 HealthSouth’s AutoAmbulator combines an overhead hoist with robotic legs to allow increased dosing of gait training even to patients with limited postural control. Again, this product is built to reduce or eliminate therapist fatigue as a limiting factor for the number of repetitions provided. When combined with a robotic exoskeleton, treadmill training has also been shown to improve left ventricular function in patients with incomplete spinal cord injury.7

Recent technologies have entered the market that enable therapists to evaluate and train visual acuity and cognitive processing as part of rehab programs. These devices can target stroke, TBI, and neurocognitive conditions.
Stationary Ergometry and Balance Technologies
Cycle ergometry can also be an effective exercise option for patients affected by neurological disorders. The 2014 AHA/ASA Scientific Statement regarding physical activity and exercise recommends stationary ergometry as a large-muscle aerobic activity for stroke survivors. The goal of physical activity for these patients is to improve functional capacity, increase independence with activities of daily living, and improve overall vascular health.5 Even patients with significant lower extremity weakness can perform cycle ergometry with the right equipment. MOTOMed devices, for example, available in the United States from EnableMe, Tampa, Fla, can provide graded levels of upper or lower extremity cycling activity—from passive, to active assistive, to resisted. They provide the patient with objective feedback regarding their performance and even have a feature that senses muscle spasms.8
For patients who regain ambulation soon after a stroke, treatment often focuses on improving gait mechanics and standing balance to improve independence and reduce risk of falls. Stroke patients who have impaired balance should participate in a balance retraining program.1 The Biodex Balance System SD from Biodex Medical Systems, Inc, Shirley, NY, is comprised of a user-controlled platform that challenges static and dynamic balance. The manufacturer claims that its use supports neuroplasticity by providing biofeedback and encouraging corrective actions in response to challenges to equilibrium. It can also provide clinicians with objective data concerning the patient’s performance.9
Measuring and Analyzing Gait
Physical therapists often focus on improving the symmetry of a patient’s gait after stroke or with other neurologic disorders. The effects of this training, however, can be difficult to objectively measure. Researchers frequently use gait mat technology, such as GAITRite, from Franklin, NJ-based CIR Systems/GAITRite, to obtain objective findings. GAITRite is a portable gait analysis system that uses sensors to provide therapists with temporo-spatial data concerning a patient’s gait pattern.10 In addition to research applications, this technology may be beneficial in the clinic to help therapists determine the efficacy of their treatment and drive changes to the plan of care.
Gait analysis technology for collecting and analyzing temporal, spatial, and pressure data is also available from ProtoKinetics, Havertown, Pa, which offers the Zeno Walkway. This device can provide utility for straight-walking and static standing assessment as well as collect data for turning, gait initiation, and gait with assistive devices such as canes and walkers.

Foot drop frequently presents as a persistent challenge for patients after stroke. Wearable technologies are available to retrain dorsiflexion during the gait cycle.
Lower Extremity Impairment
Foot drop frequently presents as a persistent challenge for patients after stroke, and is characterized by the inability to elicit the ankle dorsiflexion required to achieve adequate foot clearance in the swing phase of gait. This may vary from complete inability to elicit a contraction in the dorsiflexors, to mild weakness that causes the toe to drag more often with fatigue. Neuromuscular electric stimulation (NMES) can be used to retrain dorsiflexor activation after stroke.1 However, some patients will continue to have difficulty coordinating the dorsiflexors during gait even once a consistent volitional contraction is elicited. These patients, as well as many others, may benefit from functional electric stimulation (FES), which times the delivery of an electrical impulse to the peroneal nerve to lift the foot at the appropriate time during the gait cycle.11 The Bioness L300 Foot Drop System is one FES device commonly used for foot drop due to stroke, multiple sclerosis, and other central nervous system disorders. It incorporates an in-shoe pressure sensor that identifies when the patient’s heel strikes the ground, which signals the end of the electrical impulse.12 This technology can be used in an inpatient setting to retrain well-coordinated dorsiflexion during the gait cycle, resulting in a smoother and more efficient gait pattern. For home use, however, out-of-pocket cost to the patient can be considerable.
A patient with lower extremity weakness from stroke or other neurological disorders may benefit from an orthosis for home use. Ankle foot orthoses (AFOs) are commonly used to mechanically support a neutral ankle or to assist dorsiflexion during swing in these patients. The goal of AFO prescription may be to improve the patient’s gait pattern, reduce fall risk, or reduce the risk of orthopedic complications of hemiplegic gait. However, many therapists fear that the use of AFOs may contribute to the development of ankle contracture or muscle weakness over time. Patients without existing plantarflexion contracture may benefit from an AFO that allows ankle movement rather than a rigid AFO.13
Lewallen, et al found that patients with hemiparesis wearing a solid AFO demonstrated reduced speed when compared with an articulated AFO, posterior leaf spring, or no orthosis. The same study suggested that patients within 6 months of a stroke may benefit from the stability of a solid AFO, which could later be modified by adding articulating joints as the patient progresses.14 With so many options available, collaboration with an experienced orthotist is essential to ensure the device that is selected or fabricated will meet the patient’s needs now and in the future. Off-the-shelf and custom AFOs are available from several manufacturers, including Allard USA Inc, Rockaway, NJ which offers the ToeOFF and BlueROCKER line of products to treat foot drop, as well as the KiddieGAIT and KiddieROCKER for pediatric users.

Stroke is now recognized as a chronic condition, and recovery will be life-long for many patients. However, technologies can be used to encourage patients with stroke and other neurologic conditions to maintain an active lifestyle after discharge from therapy.
Pressure Mapping
Unfortunately, despite a therapist’s best efforts, not every person will return to walking after stroke. For individuals affected by significant neurological deficits from stroke or other disorders, it is important to maximize independence at a wheelchair level while reducing the impact of complications that can be caused by immobility. These complications frequently include infections, deep venous thrombosis, pressure injuries, loss of bone mineral density, and falls.15 Patient and caregiver education is paramount to reducing risk of these complications in the home setting. In addition, therapists must ensure the equipment that is provided to the patient is appropriate. Xsensor X3 is a pressure mapping device that can be beneficial for use in patients who are non-ambulatory or who are limited ambulators. The Xsensor ForeSite SS is designed to help clinicians analyze interface pressure data to provide patients with effective pressure redistribution. Xsensor’s pressure mapping can identify at-risk areas and reduce the risk of pressure injury, which is particularly important for patients with poor sensation. Patients with spinal cord injury, for instance, would benefit from pressure mapping during selection of an appropriate wheelchair cushion or to determine an effective strategy for pressure relief.16
Stroke is now recognized as a chronic condition, and recovery will be life-long for many patients.17 Technology can be used to encourage patients with stroke and other neurologic conditions to maintain an active lifestyle after discharge from therapy. The American Stroke Association recommends promoting engagement in leisure and recreation in addition to home or community-based exercise programs for patients after stroke.1 Smartphone apps and activity trackers can be a helpful adjunct to keep patients motivated and improve compliance with exercise and walking programs.
Reducing Risks, Raising Outcomes
Recovery of gait function and return to community function are often primary goals of rehabilitation for patients with neurologic conditions. Current advances in technology are fostering recovery from both acute and chronic neurological disorders. In many rehabilitation environments, use of technology can both enhance patient outcomes and reduce risk of injury to healthcare providers. PTP
Jessica Finnegan, PT, MPT, NCS, is the Stroke Program Manager at HealthSouth Toms River. Finnegan joined the organization in 2009 and has been a senior physical therapist since 2011. She is a board-certified specialist in neurologic physical therapy and has a focus on helping patients with stroke and other neurologic disorders return to their household and community roles. Finnegan also serves as the Physical Therapy Department’s Center Coordinator of Clinical Education and provides clinical teaching and mentorship. She earned her Master’s degree in physical therapy from Quinnipiac University. For more information, contact [email protected].
References
1. Winstein CJ, Stein J, Arena R, et al. Guidelines for adult stroke rehabilitation and recovery: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke. 2016;47(6):e98-e169.
2. Waters TR. When is it safe to manually lift a patient? Am J Nurs. 2007;107(8):53-58.
3. Darragh AR, Campo MA, Frost L, Miller M, Pentico M, Margulis H. Safe-patient-handling equipment in therapy practice: implications for rehabilitation. Am J Occup Ther. 2012;67(1):45-53.
4. Product Overviews. (n.d.). Retrieved December 11, 2016, from http://litegait.com/products
5. Billinger SA, Arena R, Bernhardt J, et al. Physical activity and exercise recommendations for stroke survivors: a statement for healthcare professionals from the American Heart Association/American Stroke Association. Stroke. 2014;45(2):2532-2553.
6. Russo A, Perret MA, Endersby K, et al. Utilization of a robotic exoskeleton to provide increased mass practice for gait training and its impact on discharge destination for individuals with acute stroke. Stroke. 47(1):1. Abstract retrieved from Ovid database.
7. Turiel M, Sitia S, Cicala S, et al. Robotic treadmill training improves cardiovascular function in spinal cord injury patients. Int J Cardiol. 2011;149(3):323-329.
8. Various accessories for an individualized training. (n.d.). Retrieved December 14, 2016, from http://www.motomed.com/en/models/motomed-viva2.html
9. Balance System™ SD. (n.d.). Retrieved December 14, 2016, from http://biodex.com/physical-medicine/products/balance/balance-system-sd
10. The validity and reliability of the GAITRite system’s measurements: A preliminary evaluation. (n.d.). Retrieved December 10, 2016, from https://www.ncbi.nlm.nih.gov/pubmed/11245768
11. Kluding PM, Dunning K, O’dell MW, et al. Foot drop stimulation versus ankle foot orthosis after stroke: 30-week outcomes. Stroke. 2013;44(6):1660-1669.
12. Help Patients Walk with More Speed, Stability and Confidence. (n.d.). Retrieved December 14, 2016, from http://www.bioness.com/Healthcare_Professionals/Exoskeletal_Products/L300_for_Foot_Drop.php
13. Mulroy SJ, Eberly VJ, Gronely JK, Weiss W, Newsam CJ. Effect of AFO design on walking after stroke: Impact of ankle plantar flexion contracture. Prosthet Orthot Int. 2010;34(3):277-292.
14. Lewallen J, Miedaner J, Amyx S, Sherman J. Effect of three styles of custom ankle foot orthoses on the gait of stroke patients while walking on level and inclined surfaces. JPO J Prosthet Orthot. 2010;22(2):78-83.
15. Let’s talk about complications after stroke. (2015). Retrieved December 14, 2016, from http://www.strokeassociation.org/idc/groups/stroke-public/@wcm/@hcm/documents/downloadable/ucm_309717.pdf
16. ForeSiteSS. (n.d.). Retrieved December 14, 2016, from http://www.xsensor.com/ForeSiteSS
17. O’neill D, Horgan F, Hickey A, Mcgee H. Stroke is a chronic disease with acute events. BMJ. 2008;336(7642):461-461.